About 23% of adults in the United States have varicose veins, but when spider telangiectasias and reticular veins are also included, the prevalence increases to 80% in men and 85% in women. Typically affecting older adults and women more frequently, varicose veins impact 22 million women and 11 million men aged 40 to 80. Among them, 2 million people, both men, and women, may experience symptoms and indications of chronic venous insufficiency, which can result in venous ulceration.
Varicose veins are a common condition that affects millions of people worldwide. They occur when the veins in the legs become enlarged, twisted, and often visible through the skin.
Varicose veins can cause discomfort and pain, sometimes leading to more severe complications such as blood clots or ulcers. While varicose veins are generally not a severe medical condition, they can be unsightly and affect a person's quality of life.
This article will discuss the symptoms, causes, and treatment options for varicose veins, as well as tips for prevention and the benefits of wearing varicose socks. Whether you are experiencing varicose veins or want to prevent them from occurring, this guide will provide you with valuable information to help you manage and understand this condition.
What is The Difference Between Spider Veins and Varicose Veins?
Spider veins and varicose veins are two common types of vein disorders that can occur in the legs. While they are both caused by problems with the veins, there are several differences between the two conditions.
Spider veins, also known as telangiectasias, are small, thin veins that are visible just under the surface of the skin. They typically appear as a web-like pattern of red, blue, or purple lines and are most commonly found on the legs or face. Spider veins are generally not painful or harmful, but they can be unsightly and may cause discomfort or itching.
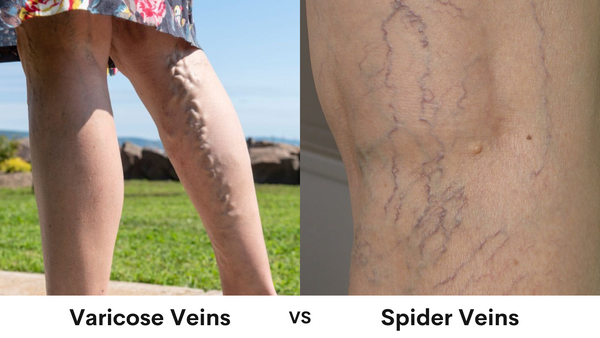
Varicose veins, on the other hand, are larger, bulging veins that are twisted and rope-like in appearance. They can be painful and may cause aching, heaviness, or swelling in the legs. Varicose veins are caused by weakened or damaged valves in the veins that allow blood to flow backwards and pool in the veins, leading to their enlargement.
While spider veins and varicose veins have different causes and symptoms, they can often occur together. In fact, spider veins are sometimes a sign of underlying varicose veins. Both conditions can be treated with a variety of medical and lifestyle interventions, depending on their severity and underlying causes.
Symptoms and Causes of Varicose Veins
Varicose veins can cause a range of symptoms and may be caused by several factors. Here are some of the most common symptoms, risk factors, and causes of varicose veins:
Symptoms of varicose veins:
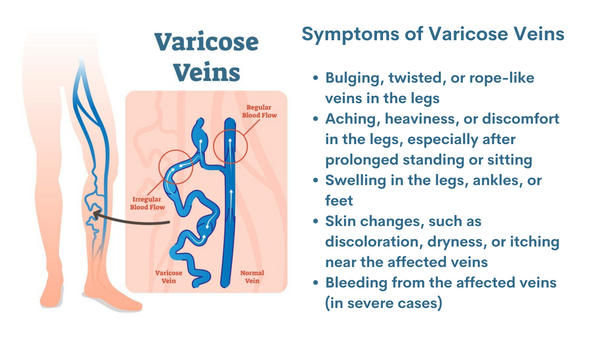
- Bulging, twisted, or rope-like veins in the legs
- Aching, heaviness, or discomfort in the legs, especially after prolonged standing or sitting
- Swelling in the legs, ankles, or feet
- Skin changes, such as discolouration, dryness, or itching near the affected veins
- Bleeding from the affected veins (in severe cases)
Risk factors for developing varicose veins:
- Age: Varicose veins are more common in older adults, as the veins become weaker and less elastic with age.
- Gender: Women are more likely to develop varicose veins than men, likely due to hormonal changes during pregnancy, menopause, or the use of birth control pills.
- Family history: If other family members have varicose veins, you may be more likely to develop them as well.
- Obesity: Excess weight puts extra pressure on the veins in the legs, increasing the risk of varicose veins.
- Prolonged sitting or standing: Jobs or activities that require long periods of sitting or standing can increase the risk of varicose veins.
Causes of varicose veins
- Weak or damaged valves: The veins in the legs have one-way valves that help the blood flow towards the heart. When these valves weaken or become damaged, blood can flow backwards and pool in the veins, leading to their enlargement.
- Genetics: Some people may be born with weaker vein valves or have a family history of vein disorders that increase their risk of developing varicose veins.
- Pregnancy: The increased pressure on the veins in the pelvis and legs during pregnancy can lead to varicose veins.
- Injury: Previous leg injuries or surgeries can damage the veins and lead to varicose veins.
Understanding the symptoms and causes of varicose veins can help you identify and manage this condition. In the next section, we will discuss when to worry about varicose veins and seek medical attention.
When to Worry About Varicose Veins?
While varicose veins are generally not a serious medical condition, there are some cases where they may indicate a more serious underlying issue. When varicose veins may be a sign of a more serious condition:
- Deep vein thrombosis (DVT): Varicose veins can increase the risk of developing blood clots in the deeper veins of the legs, known as DVT. This condition can be life-threatening if left untreated.
- Venous ulcers: Long-standing varicose veins can cause skin damage and lead to ulcers (open sores) on the skin near the affected veins.
- Bleeding: In rare cases, varicose veins can bleed and cause significant blood loss.
When to seek medical attention:
- Severe pain or swelling in the legs
- Skin changes or ulcers near the affected veins
- Bleeding from the affected veins
- Difficulty walking or standing due to the pain
- Signs of infection, such as redness, warmth, or tenderness around the affected area
If you are experiencing any of these symptoms, seeking medical attention as soon as possible is important. Your healthcare provider may recommend a range of treatments, including compression stockings, lifestyle changes, or in some cases, surgery.
In the next section, we will discuss some of the best treatment options for varicose veins.
Varicose Veins Treatment Options
Varicose veins can be managed with a range of treatment options, from conservative methods to medical procedures. Here are some of the most common varicose veins treatment:
Conservative treatments for varicose veins:
- Exercise: Regular physical activity, such as walking or cycling, can improve blood circulation and help prevent varicose veins from getting worse.
- Compression stockings: These specially designed stockings provide gentle pressure on the legs, promoting blood flow and reducing swelling.
- Lifestyle changes: Simple lifestyle changes, such as maintaining a healthy weight, elevating the legs when resting, and avoiding prolonged sitting or standing, can help manage varicose veins.
Medical treatments for varicose veins:
- Sclerotherapy: This procedure involves injecting a solution directly into the affected vein, causing it to close and eventually fade away.
- Endovenous laser treatment (EVLT): This procedure uses a laser to heat and close off the affected vein, which is then absorbed by the body.
- Surgery: In some cases, surgery may be necessary to remove the affected veins. This is typically reserved for severe cases or if other treatment options have failed.
The best treatment options for varicose veins based on severity and other factors:
The best treatment for varicose veins will depend on the severity of the condition, as well as individual factors such as age, overall health, and personal preferences.
Mild cases of varicose veins may be managed with conservative methods such as exercise and compression stockings, while more severe cases may require medical treatment. It is important to consult with your healthcare provider to determine the best course of treatment for your varicose veins.
In addition to treatment options, there are also preventive measures that can be taken to reduce the risk of developing varicose veins or prevent them from getting worse.
In the next section, we will discuss some tips for preventing and managing varicose veins.
How to Get Rid of Varicose Veins Naturally?
While medical treatments for varicose veins can be effective, some people may prefer to try natural remedies first. Here are some natural remedies that may help alleviate the symptoms of varicose veins:
Natural remedies for varicose veins:
Essential oils
Certain essential oils, such as lavender, chamomile, and peppermint, have anti-inflammatory properties and may help reduce swelling and pain associated with varicose veins. They can be applied topically to the affected area or added to a warm bath.
Diet
Eating a healthy, balanced diet that is rich in fibre and antioxidants can help improve blood flow and reduce inflammation. Foods that are high in vitamin C, such as citrus fruits and leafy greens, can also help strengthen the walls of the veins.
Herbal supplements
Certain herbs, such as horse chestnut and butcher's broom, have been traditionally used to improve circulation and reduce swelling. They are available in supplement form and should be used with caution, as they may interact with certain medications.
Effectiveness of natural remedies for varicose veins:
While natural remedies may provide some relief for the symptoms of varicose veins, it is important to note that there is limited scientific evidence to support their effectiveness. It is always recommended to consult with a healthcare provider before trying any new treatments or supplements.
It is also important to note that natural remedies should not be used as a substitute for medical treatment in cases of severe varicose veins. In some cases, medical treatment may be necessary to prevent complications or further damage to the veins.
Varicose Veins Prevention
While varicose veins may be a common condition, there are steps you can take to reduce your risk of developing them or prevent them from getting worse.
Tips for preventing varicose veins:
- Maintain a healthy weight: Being overweight or obese puts extra pressure on the veins in the legs, increasing the risk of developing varicose veins.
- Stay active: Regular physical activity, such as walking or cycling, can help improve blood circulation and prevent varicose veins from getting worse.
- Avoid prolonged sitting or standing: If you have a job that requires you to sit or stand for long periods of time, take breaks to move around and stretch your legs.
- Elevate your legs: Elevating your legs above the level of your heart can help improve blood flow and reduce swelling.
- Wear compression stockings: Compression stockings provide gentle pressure on the legs, promoting blood flow and reducing swelling.
How to reduce the risk of developing varicose veins:
In addition to these tips, there are also lifestyle changes you can make to reduce your overall risk of developing varicose veins:
- Wear sunscreen: Sun damage can weaken the skin and increase the risk of developing spider veins, which can progress to varicose veins.
- Avoid tight clothing: Tight clothing, particularly around the waist, groin, and legs, can restrict blood flow and increase the risk of developing varicose veins.
- Eat a healthy diet: A diet that is high in fiber and antioxidants can help improve blood flow and reduce inflammation, reducing the risk of developing varicose veins.
By incorporating these tips into your daily routine, you can help prevent varicose veins from developing or getting worse. If you are concerned about varicose veins, talk to your healthcare provider to determine the best course of action for your individual needs.
Varicose Veins Exercise
Exercise is an important component in the prevention and management of varicose veins. Regular physical activity can help improve blood flow, strengthen the muscles that support the veins, and reduce swelling in the legs. Here is what you need to know about exercise and its effect on varicose veins:
Exercise And Its Effect On Varicose Veins:
Exercise helps to improve blood circulation and can prevent blood from pooling in the veins. This, in turn, can reduce the likelihood of varicose veins forming or getting worse. Exercise can also help to strengthen the muscles that support the veins, reducing the pressure on the veins and preventing them from becoming enlarged.
Types Of Exercises That Are Beneficial For Preventing And Reducing Varicose Veins:
- Walking: Walking is a low-impact exercise that can help improve blood circulation in the legs. It is a great option for people of all fitness levels and can be done almost anywhere.
- Cycling: Cycling is another low-impact exercise that can help improve blood circulation in the legs. It can be done on a stationary bike or outdoors and is an excellent choice for people who are looking for a low-impact form of exercise.
- Swimming: Swimming is an excellent option for people who want to exercise without putting any pressure on their joints. It is also an excellent way to improve blood circulation and reduce swelling in the legs.
- Yoga: Doing Yoga can help improve blood circulation, reduce stress, and increase flexibility. Certain poses, such as the Legs-Up-the-Wall pose, can also help to reduce swelling in the legs.
- Strength training: Strength training exercises, such as squats and lunges, can help strengthen the muscles that support the veins in the legs, reducing the pressure on the veins and preventing them from becoming enlarged.
Varicose Socks
Varicose socks, also known as compression stockings, are a type of hosiery designed to improve blood flow in the legs and prevent or manage varicose veins. Here's what you need to know about varicose socks:
What are varicose socks?
Varicose socks are specially designed stockings that apply pressure to the legs, helping to improve blood flow and prevent blood from pooling in the veins. They are available in different compression levels, lengths, and colours, and can be worn by both men and women.
How do they work?
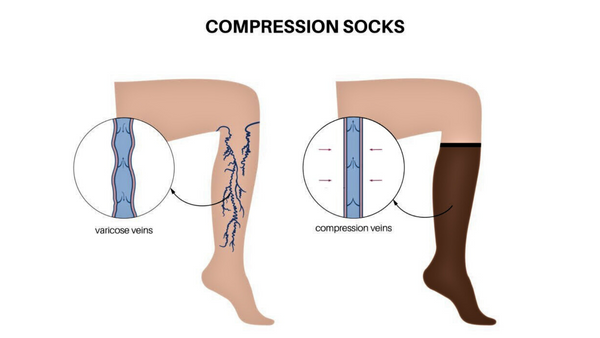
Varicose socks work by applying pressure to the legs, which helps to improve blood circulation and prevent blood from pooling in the veins. They are designed to be tightest around the ankle and gradually become less tight as they go up the leg. This gradient compression helps to push blood back up towards the heart and prevents it from pooling in the veins.
The benefits of wearing varicose socks
Preventing and managing varicose veins: Varicose socks are a non-invasive and effective way to prevent and control varicose veins. By improving blood flow in the legs, they can reduce the risk of developing varicose veins or prevent existing varicose veins from getting worse.
- Reducing leg swelling: Varicose socks can help reduce leg swelling by improving blood flow and preventing blood from pooling in the veins.
- Relieving leg pain and discomfort: Varicose socks can help reduce leg pain and discomfort by improving blood circulation and reducing the pressure on the veins.
- Promoting healing after surgery: Varicose socks are often recommended after surgery to prevent blood clots and promote healing.
Varicose socks can be purchased over-the-counter or prescribed by a healthcare provider. It is important to choose the right size and compression level to ensure the best results. It is also important to wear them properly, putting them on in the morning before getting out of bed and taking them off at night before going to bed.
Final Thoughts
From lifestyle changes and exercise to medical treatments and compression stockings, there are many ways to improve blood flow and reduce the appearance of varicose veins. It's important to take action if you experience symptoms of varicose veins or have a family history of the condition. With the right treatment plan and preventative measures, you can help keep your legs healthy and pain-free. Remember to always consult with your healthcare provider before starting any new treatments or exercises.
























































